The answer to this question is not as straightforward as you might think and even doctors get it wrong sometimes. Proper diagnosis is important because treatment can take a long time, can be expensive, and may be associated with certain side effects. If you suspect you have a nail fungal infection, you should know the symptoms of nail fungus(onychomycosis) and make sure that your physician performs the proper diagnostic tests.
Onychomycosis, or a nail fungus infection, is defined as a fungal infection of the nail bed, nail plate (what we think of as the nail itself) or the area very closely surrounding the fingernail or toenail. Most cases of nail fungus are caused by a dermatophyte called Trichophyton rubrum. Many other cases are caused by Candida albicans, which is a yeast. These organisms can invade deeply into the nail or stay near the surface. They can begin their infection process near the cuticle or at the tip. (Nail Fungus under a microscope)
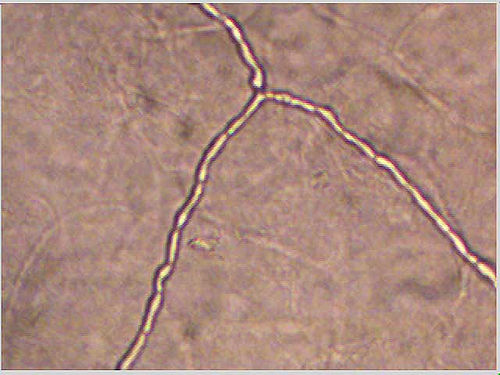
Onychomycosis is responsible for one third of all fungal skin infections and half of all nail infections. Even so, that means that half of all nail infections are not caused by fungi. Therefore it is important to distinguish between a nail fungus and a bacterial infection of the nail. A fungal infection is treated with an antifungal while a bacterial infection is treated with an antibiotic.
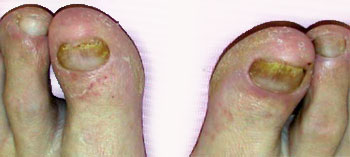
Fungal nail infections can cause a number of abnormalities in the nail. Almost all cases of nail fungus will include white, yellow, or white-yellow crust in or on the nail. This is the fungus itself. The white-yellow patches can be in the form of streaks that are parallel to the finger. Alternatively, the lesion can appear across the tip or the cuticle. When the crust spreads, it can cover the entire surface of the nail.
If the fungus penetrates underneath the nail plate (the nail itself), which is often does, it can form irregularities in the nail bed. The bumpy nail bed is less able to hold onto the nail and so it becomes loose. Since dermatophytes consume keratin and produce destructive wastes, the nail can become pitted and misshapen. This may cause ridges and grooves in the nail.
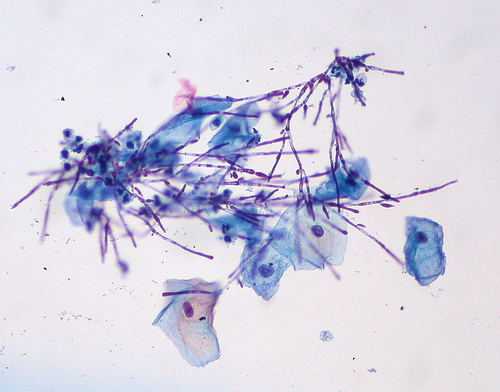
If the nail fungus infection becomes severe or contains Candida, the nail folds and skin surrounding the nail may become red and swollen. These are signs of inflammation which can cause discomfort and even pain. The skin may express (ooze) pus, which is a whitish material common of white blood cells from the immune system.
Pus is usually a sign of bacterial infection and, if it is present, may be a “red herring” for the physician trying to make the diagnosis.
A nail that is expressing pus may be assumed to be caused by a bacterial infection, as is often the case. If you are experiencing pus it is particularly important to get a correct diagnosis for the nail infection. In addition to bacterial nail infection, there are a number of diseases that can mimic a nail fungus. Examples of mimickers include hallopeau acrodermatitis, lichen planus, nail bed melanoma, nail bed psoriasis (may occur with fungal infection of the nail), onycholysis, paronychia, Reiter syndrome, or yellow nail syndrome. This means that one or more diagnostic tests are necessary to make the correct diagnosis of onychomycosis.
Testing for a nail fungus requires that a piece of the diseased nail be taken for further study and analysis. If the disease affects the tip of the nail, like in distal subungual onychomycosis, a small piece of nail can be trimmed from the end. Unfortunately in proximal subungual onychomycosis the nail must be removed down to the base. On the positive side, this nail removal can be therapeutic as well as diagnostic. In white superficial onychomycosis, the lesion is scraped away from the top of the nail.
Once a piece of the diseased nail is harvested, two main tests are performed on the sample. Some of the nail can be treated with a strong base, namely potassium hydroxide, and viewed under a microscope for the presence of fungi. The remaining piece of nail can be sent for a fungal culture. The sample is placed in an environment in which fungus can grow and thrive and, after a few days, the sample is checked for growth of new fungus. The presence of fungus in one or both of these tests is good evidence that an onychomycosis is present. If neither the potassium hydroxide wash nor the culture show fungus, the nail can be taken, pulverized, and sent to a pathologist for analysis. Alternatively a portion of the nail can be sent for a bacterial culture in case the nail infection is not fungal.
If you suspect that you have nail fungus symptoms, the diseased nail or nails should be looked at by a physician, ideally a dermatologist. Proper diagnosis of the illness is important for directing care and ruling out for serious problems.
References
Hainer BL. Dermatophyte infections. Am Fam Physician 2003;67:101-108.
Jaffe R. Onychomycosis: recognition, diagnosis, and management. Arch Fam Med 1998;7:587-592.
Kaur R, Kashyap B, Bhalla P. Onychomycosis–epidemiology, diagnosis and management. Indian J Med Microbiol 2008;26:108-116.
Click Here For Highest Rated Nail Fungus Treatments
1. Funginix - www.Funginix.com
2. Zetaclear - www.Zetaclear.com
3. PurNail - www.Purnail.com

Anna Reed says:
My toenail has not turned yellow. It has pulled away from the nail bed on the top 1/3 re of the nail. There is a while semi hard matter under the nail. If I try to remove it , it will bleed a lot and be hard to stop. The nail looks raised and rounded looking instead of flat. Now my fingernail have been brittle, peal and crack . They are white and flat but I have tried vitamins and other things. I asked toe Dr., Pharmasist and no one knows what vitamin or mineral might help.
Janette Marshall says:
Quite a lot of toe nail skin infections are bacterial. Think about it, our feet are just as prone to picking up infections as any other part of our bodies. Try soaking feet in a bowl of warm fresh water and honey, only a very good grade honey. Honey eats away at all bacterial infections very quickly clearing them up. Do this daily if you need to and dab a little neat honey on the infected area before bedtime or during the day and wear a pair of clean socks each day.
Anna says:
Anna,
My toenail is the same and I haven’t found an answer yet.
I am going to try the honey and then the tea tree oil!
Did yours clear up? What did you find worked best?
David Whitney says:
judging by your description, i do think toenail fungus is what i have. i
thought it’s just a stain, or my nail became dead. i haven’t felt
anything in them yet nor pus lesions, or dry skin.only a yellow nail. am
i supposed to take meds at this moment?would you know the right treatment i
should take?thank you.
dina lopez says:
hello, my name is dina my toenail recently separated from the nail bedbed is not completly yellow but has soom discolorment…I am a runner and awhile back my nail was hurting because it was to long. Now im not sure if i have funges or if it is for the 2nd reason.. and should i take off the nail or let the new one grow out with it. my nail is pretty thick compared my other toenail.
holly werlwas says:
After reading this article, it would seem as though a doctor had all the answers. I have what I believe is a toenail fungus. I have been to my family doctor, who referred me to a foot dr., and finally a dermatologist. I can assure you, none of these doctors even do half of what this article says they should do. In fact, 2 drs. looked very briefly at my feet and told me to go get some of the stuff from the drugstore. The dermatologist gave me a prescription for lamisil only after I asked for it. Turns out I am probably allergic to it and can’t take it anyway. But if anyone knows of a doctor as conscientous as the fictional one above… please give me his or her name! I am tired of being charged ridiculous amounts of money for doctor visits that are useless.
Dana says:
I thought I had toenail fungus for a while (yellow, separating from nail bed), and I finally went to my dermatologist. He took one look at my nail and said he didn’t think it was fungus, because the nail wasn’t thickening. He looked at some trimmings under the microscope to be sure, but in the end determined it was a bacterial infection (pseudomonas, the same that causes swimmers’ ear) which is contracted in the same way that one would get a fungal infection. The treatment ended up being really easy, I just had to soak my feet in a solution of 1 cup warm water, 2 tablespoons white vinegar for 10 minutes, twice daily. And it worked! It is really important to trim your nails as short as possible, and make sure to rinse and dry them really thoroughly. The infection is cleared up, but I still do the soaks everyone once in a while to make sure it doesn’t come back.
Also, in response to an above comment, it’s really important not to dig and poke under your nail, because it can damage the nail bed so your nail doesn’t grow back properly, and can introduce infection if you don’t already have one!
lynn says:
I’ve had a nail fungus for six months its cleared up. I used tea tree oil. I would put my finger in the bottle and pour it on my nail. I did this twice a day then at night I would pour it on my finger then soak a piece of paper towel and tape it to my finger while I slept. Its not comfortable sleeping with the smell but it works.I’ve done this process for the last two weeks and has helped dramatically. Its gone. I will continue to put it on for another week or two just so its completely gone..Ladies DO NOT WEAR NAIL POLISH AT ALL.!!!
Elda says:
My baby is a year old and her big toe najl is white and very thick and looks infected, wat advice do yall have besides a dr, all he said was to let it grow out…..and its still the same
Rita says:
I had a terrible reaction to years of wearing fake salon nails.
I had green black under and by the time you notice its really bad mold green.
You have to remove the nails, If its is painful. Soaking in salt water is good. The vinegar, listerine is also good when its gotten this bad and probably good Idea to see you GP or dermatologist. I then applied an antibotic cream religiously, buy a few so you have them handy.
Rubbing alcohol is also a great way to dry it out.
You have to buff the nail with a 4 way nail file and get it as flat as you can after soaking it will become soft so you won’t be dramaging you nail to much. I think staying away from nail salons is you best bet.
Once you have gotten to this stage, I apply Vitamin E or A oil Religiously. Everytime you can but, at nite its a must.
I then bought some Sally Hansen products for nails mostly the tea tree or fast growth in 5 to 7 days. I has spent so much on fake nails over 40 years this was way cheeper.
I was so discussed with my nails my toes were fine but, this problem jumps to other nails fast if you don’t stay on top of it.
I met a friend who suggested using Nail TEK. A polish to put on your nails repeatedly and then remove.
My son was gettin married in a year and thought I am going to grow my own long nail for the Wedding, My motivation!
I also was told by his fiance to buy Sally Hansens Hard as Nails. So I also did that.
But, I think what speeded up the process was I started taking fish oil, vitamin E, vitamin D, vitamin C and stopped taking any medication. I was on Boniva and I think it had something to do with this in my system. Eat fruit, vegetables, n fish.
I know this is a combination of several things in which you should try all. NO side effects………. from these.
I must add that I was watching DR, OZ and a segment of nails and it was suggested to place some garlic juice in your nail polish and paint it on your nails.
I got an old nail polish bottle that had oil in it I mixed the juice from a jar of store bought chopped garlic and vitamin E oil.
I leave this on the counter and when ever I sit there I polish it on, The garlic does not smell. I started last July with this and my nails are strong and long. I have to cut them. I put this on my toes too. They are much better. Also filing your nails and buffing with a metal file one way not back and fourth. Using as I mentioned a soft 4 way file that way your nails will look more natural always apply the vitamin E oil after filing and put a coat of your nail tec once all signs of infection are gone.
I have that calis under a right thumb and pick at it and my nails were nice but I started digging at it and made a gap under the nail same problem I had with fake nails picking creating this problem. So then I noticed it began to turn green with fungus oh S…………….T. Here we go again, I think we are our own distructors when it comes to treating our nails. So you have to cut the nail back and the uglyness that is created so quickly this discuss me and I caused it.
So I thought I have to get a quick remedy! I been so good about not picking… well, I had that wedding well thats over! So I guess I took it out on that one nail. I did Hydro peroxide not always the best but it does clear up any initial infection especially when it starts bubbling. I sprayed windex and saw that someone mentioned soaking in diluted bleach well, I had Soft scrub under the sink. I put a little in a cup with water and a Qtip this was yesterday applied it and the green on my nails started to fade. I guess mold in bathrooms you kill it with bleach so what the heck it was handy and its like bleach well this morning its almost fadded completely. However, I would make sure you have NO signs of open cuts… this not something I would recommend and test a small area first to sense if there is any pain. I had none when I applied left on for 10 seconds and rinsed and dryed. I applied Vitamin E oil to nail. I left it alone and open however, its good to keep your nails dry even if you have to get a blow dryer on low heat to dry out the nail digging under the nail is what I did because I just couldn’t stand looking at it so I did some drastic measures so that the mold green was gone. Lesson, don’t pick or dig underneath the nail bed to create little pockets of moisture to seep in and get trapped causing this a happy haven for fungus to grow. Keeping your hands free from dampness where gloves, I have them everywhere. Its really temping to wet your hands all the time. I buy a box of a 100 without the powered inside or playtex gloves by your sink. Once you begin to use these product which ever suits your budget but, the days of fake nails are over short natural painted nails are what is the fashion now. Check out my favorite on I heart Radio performance of Carrie Underwood. Check out her nails Just beautiful natural clean and clear. Its also said that Lemon juice makes your nails white. I bought a polish from Sally Hansen Whiter NaIls its clear used it religiously also, first coat. But, all the natural remedies are good if you are on a beer budget. I know that getting your nails to a healthy state takes a year if you follow these tips. These tips now from painfull expierence and getting it in your head no one really notices your nails when they look nice only when they look infected or green. I will never wear any kind of green color polish because it reminds me of fungus!!!
Get soaking, get oil, take vitamins, don’t pick at them and do not attend any salons. When you start seeing results by just the oil and garlic you kick yourself for spending all that money in the salon which is probably where you got the fungus if you never had it before or you may have the Candita? and you would need to see the doctor for that however, I did and they gave me a tube of Cutemol a sample tube last a good six months if you use often. It is very concentrated. You can get this thru Amazon if your Dermatologist is not handing out samples and Derma Nail, two items that initially helped with the infection, I also carried a cuticle pen another Sally Hansen product this conditions your cuticles are dry or cracking especially at work or travel great handy thing to have smells good. Sorry I know this is alot of stuff but, let me save you the trouble of figuring it out what will get rid of this ugly problem. Mine from fake nails and pick causing my own problems. But, internally I had some stuff going on but with in the year its amazing how long and strong they have gotten and getting rid of the old nail now that the bottom of your nail since the bed is a new nail now. Keep them short which is hard cuz now their your nails and why on god green earth would I want to cut them shorter well they wiill be stronger. I didnt so they are now breaking but, I have not been as religious and slacked on wearing gloves cleaning, doing yard work puts alot of strain on the tips of your figure nails when they are still getting strong. So patience is the key and keeping this stuff applied. I so want to get a mani pedi at a spa salon but, again its proven time and time again the tools are not clean and the pedi stations are not either and if you are sensitive it can create worse problems for feet toes and legs.
Good luck on clearing up the fungus problem but, I today I am looking at a clear nail after yesterday a nail that looked like it got smashed in a door. I truely believe that putting the soft scrub did the trick instantly. But now the nail is a half and inch below the top of my thumb and willl probably take 3 or 4 month to get back to the tip of my thumb. boo!! I have only 4 nails out of 10 that have not fully grown to the tip of the nail and thats because they tore at the corner and I had to start again the difference is the nail is thicker and try not to file the nail too thin the nail salons did a good job with that drilling all the time and thinning. Cuticles and the upper bottom corners of nails are the areas that stimualte grown so try not to dig into those areas until you see signs of growth. Aloha!!
Rita says:
plz forgive my typos wish there was a spell check!
marlee says:
I have only on my big toes this infection. My doctors say it is a fungus. I am on lamisil right now, just to see if it will work. The person who said they got the nail fungus from a salon well the place you went to is not sanatizing their equipment. I get my nails down once in a while and have not had a problem.
Emily says:
So I have brown stuff on my toenail. It was on my big toe one day and I thought I had just stubbed my toe and didn’t remember, but the next thing I know it’s on 2 other toes and then my other foot!